
Sometimes patients and parents choose not to vaccinate1
Understanding the motivation behind their decisions can help you formulate a plan.2-5
The World Health Organization estimates that vaccination saves 3.5-5 million lives worldwide every year.6 Despite the availability, many still delay or refuse recommended vaccines, which can lead to outbreaks of vaccine-preventable diseases.2,3
This choice is often attributed to a lack of confidence in vaccine efficacy and safety; however, studies show there are three main motivating factors that may influence vaccine hesitancy3-5:
Factors That Influence Vaccine Hesitancy4,5
Convenience
- Ease of physical access, affordability, and availability
- Understanding of vaccination services
Confidence
Trust in:
- Effectiveness and safety of vaccinations
- Vaccination delivery systems
- Motivations of decision-makers
Complacency
- Low perceived risk of vaccine-preventable diseases
- Under-appreciation and deprioritization of vaccination

Talk with your patients to determine the exact cause for their hesitancy and address accordingly.
SDOH influence parental decisions about vaccination7
In data from the 2018-2019 NIS-Child Survey, 23.6% (n=1804) of parents with children aged 19-35 months reported hesitancy toward childhood vaccinations.7,a
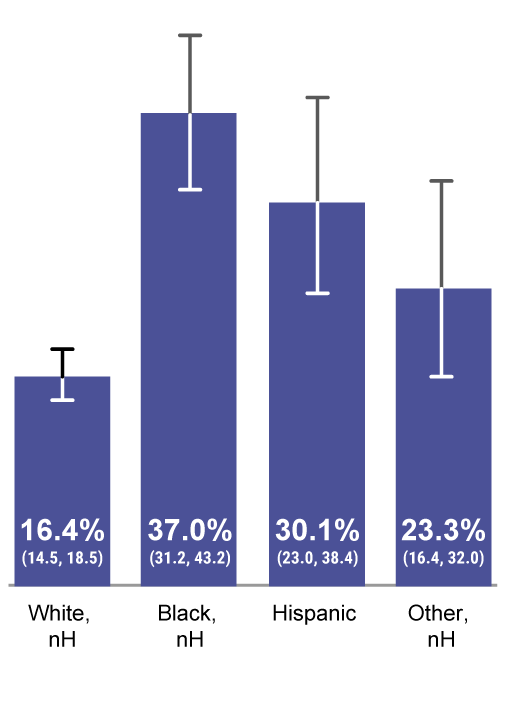
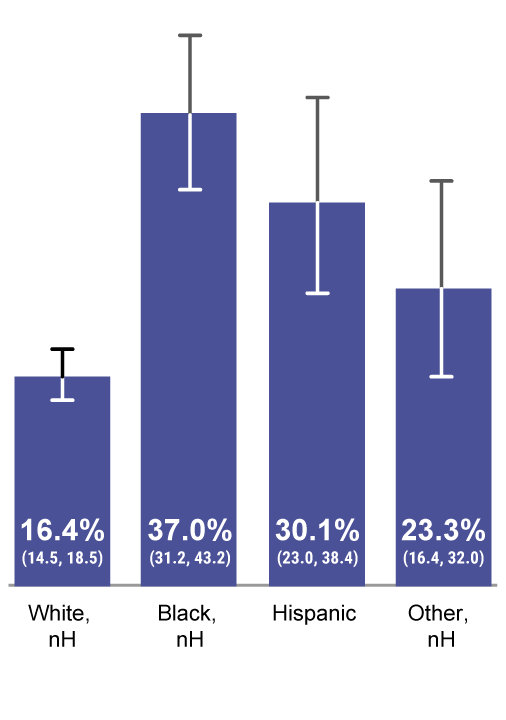
Parental vaccine hesitancy differed by race/ethnicity, mother’s education level, and poverty status.7,a
Percent of Parents Reporting Hesitancy7,a
Child’s Race/Ethnicity
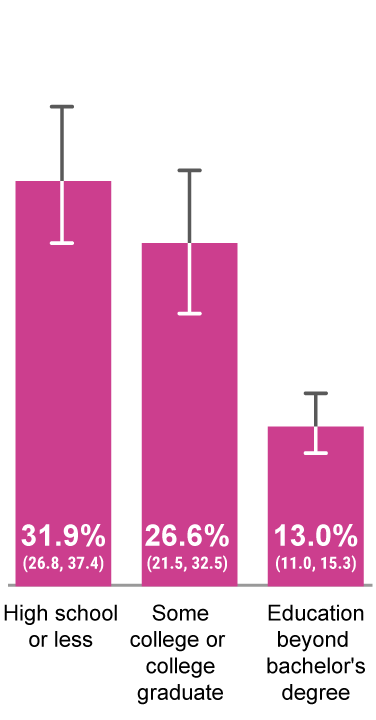
Mother’s Education Level

Poverty Status
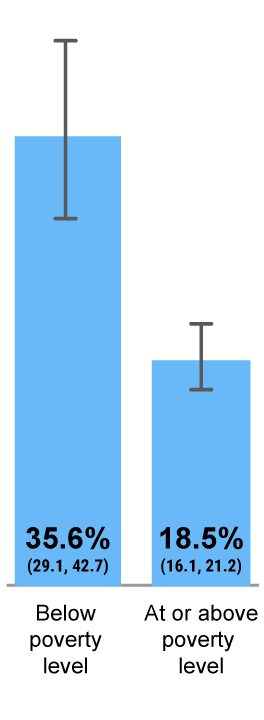
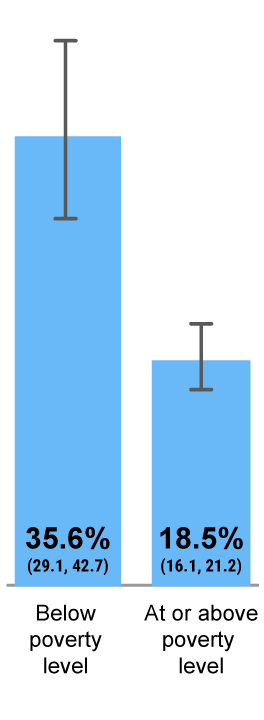
Among the hesitant parents, vaccine hesitancy contributed to approximately 15%–25% of undervaccination among children aged 19-35 months7,a
aNIS-Child is an annual, random digit-dialed telephone survey conducted by the CDC among parents or guardians of children aged 19–35 months. The association of parental vaccine hesitancy with vaccination coverage was assessed using a CDC-developed 6-item questionnaire where parents were asked questions on their perceptions of childhood vaccination. Data were collected for 14,077 children.7
CDC, Centers for Disease Control and Prevention; nH, non-Hispanic; NIS, National Immunization Survey.
Be prepared for honest conversation
Explore scientifically proven techniques for overcoming vaccine hesitancy and communicating effectively with parents.
Learn more about hesitancy and how to address it
References
- Centers for Disease Control and Prevention. Talking with parents about vaccines. Published August 9, 2024. Accessed November 1, 2024. https://www.cdc.gov/vaccines-children/hcp/conversation-tips/index.html
- Talbird SE, Carrico J, La EM, et al. Impact of routine childhood immunization in reducing vaccine-preventable diseases in the United States. Pediatrics. 2022;150(3):e2021056013. doi:10.1542/peds.2021-056013
- Kempe A, Saville AW, Albertin C, et al. Parental hesitancy about routine childhood and influenza vaccinations: a national survey. Pediatrics. 2020;146(1):e20193852. doi:10.1542/peds.2019-3852
- MacDonald NE; the SAGE Working Group on Vaccine Hesitancy. Vaccine hesitancy: definition, scope and determinants. Vaccine. 2015;33:4161-4164. doi:10.1016/j.vaccine.2015.04.036
- Allen A, Butler R. The challenge of vaccination hesitancy and acceptance: an overview. In: Meeting the Challenge of Vaccination Hesitancy. The Sabin-Aspen Vaccine Science & Policy Group; 2020;48-86. https://www.sabin.org/app/uploads/2022/04/Sabin-Aspen-report-2020_Meeting-the-Challenge-of-Vaccine-Hesitancy.pdf
- World Health Organization. Vaccines and immunization. Accessed September 10, 2025. https://www.who.int/health-topics/vaccines-and-immunization#tab=tab_1
- Nguyen KH, Srivastav A, Lindley MC, et al. Parental vaccine hesitancy and association with childhood diphtheria, tetanus toxoid, and acellular pertussis; measles, mumps, and rubella; rotavirus; and combined 7-series vaccination. Am J Prev Med. 2022;62(3):367-376. doi:10.1016/j.amepre.2021.08.015